Researchers Make Some Noise with a Silent Stroke Tool
April 2019
In the time it takes to read the few paragraphs of this story, somewhere in the U.S., a person will suffer a stroke. That's roughly every 40 seconds. At the University of Nebraska—Lincoln, Steven Barlow's research team is developing solutions for front-line treatment after a stroke. It's all a question of blood flow.
One of the most common strokes is termed "ischemic stroke." It obstructs blood flow to the brain, depriving it of the oxygen it needs to survive. Ischemic stroke is the leading cause of long-term disability and fifth-leading cause of death in the U.S.
"They have this phrase in the stroke literature, ‘time is brain.' Every minute, you lose approximately 2 million neurons and 14 billion synapses as the stroke evolves," said Barlow.
Using brain imaging, Barlow and his colleagues have found that their technology can increase brain blood flow up to 20 percent. In animal studies, it forced the brain to reroute blood supply to affected areas, to protecting the cells. Technically speaking, the science is a pTACS somatosensory stimulator, which is paired with a fixation device for functional transcranial Doppler ultrasound.
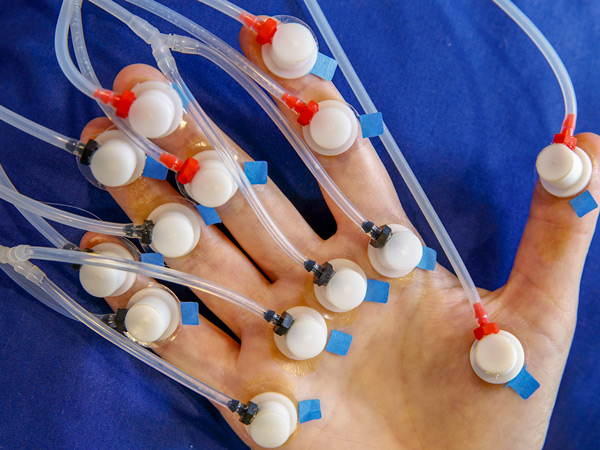
At first glance, the setup appears as complex as its name. There's a headband that stretches across the wearer's forehead, plus a spattering of white capsules stuck to their hands with clear plastic tubes sticking out. Pressurized air is pumped through the tubes, into the white capsules, and creates blood flow stimulus to the brain. As complicated as it looks, the treatment is non-invasive. And operationally silent. It's a novel solution for a hectic emergency room, not the least because it could accelerate patient recovery from the get-go.
"It's hard to overstate the impact this could have."
The team is now partnered with CHI Immanuel Medical Center in Omaha to bring the technology to clinical trials with stroke patients. "When you think about the number of stroke victims, and it spans all ages, it's hard to overstate the impact this could have," said Barlow's fellow researcher Greg Bashford.
And with the continued support of the University of Nebraska resources, one can only imagine the impact they'll make.
Pictured in the header photo, from left to right: Doctoral student Jacob Greenwood, researchers Steven Barlow and Greg Bashford, doctoral students Ben Hage and Elizabeth Hoffman.
Discover our Podcast Series
The “Leading Nebraska” podcast shares the stories of the researchers, students, teachers and others across the University of Nebraska's four campuses who are making an impact. From teachers and doctors to engineers and ag experts, these Nebraska leaders are touching lives and making a difference.